Do you believe your organization has too many performance measures or too few? Having good data available enables better decisions to be made, but not when the expense of collecting all the data is so high that it severely limits your resources to fix problems and improve quality. This results in a lot of measuring, but rarely a chance to make the cut.
If asked if you believe your organization has too many different measures or too few, how would you answer?
a) We have way too many metrics, but they all provide valuable information
b) We have too many metrics and they don’t provide the information we need
c) We have just the right amount of metrics to balance the need for information and action
d) We have too few metrics to adequately measure performance
If you answered “c,” then you are among those who have implemented a performance management system that truly works for the entire organization. Sometimes we only have the resources to track required measures like CMS Core Measures. Or, we might track so many different measures that at time we believe we are some kind of data manufacturing company instead of a hospital. In this case, it feels like more time is spent compiling data and reports than actually working on improvement projects.
So, what are the characteristics of a good performance measurement system?
The system must be designed as a tool for tracking financial results while simultaneously monitoring the system’s capabilities to meet customer needs, key performance indicators, and critical success factors.
At the executive level, the system represents the acme of a hierarchy of indicators that, ultimately, reach both the bedside and the loading dock. Ideally, each employee knows how his or her work impacts the uppermost corporate indicators. Given these considerations, many organizations seek to implement the balanced scorecard.
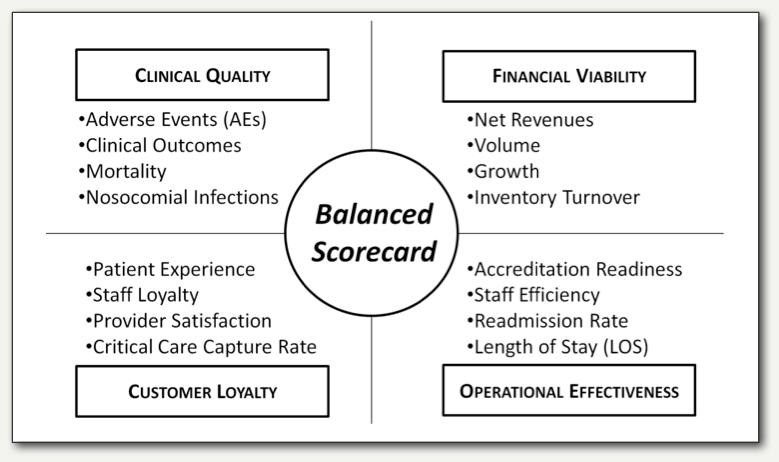
Although the balanced scorecard represents a vision and a benchmark for measuring performance in an organization, the first step is beginning to design effective performance measures. Here are some things to think about when doing just that:
- Indicators are specific. A hierarchy of metrics links layers of accountability so that staff at every level of the organization are measured on their contribution to metrics at the highest level. There is a clear line of sight upward, from each worker’s job to the executive dashboard and from the dashboard down to division and departmental indicators and the specific activities moving the dial.
- Indicators are logical and based on clear operational definitions. process capability and performance against objectives is quantifiable.
- Indicators are actionable. performance improvements can be linked directly to changes in performance indicators
- Indicators are relevant. Everything that matters (the critical few indicators defined by organizational strategy) is measured and nothing more.
- Indicators are related to time. Performance over time (trending) is evident and key processes are measured frequently enough to allow for timely corrective action.
As we work towards moving our organizations to “answer c,” the effort will certainly require a collaborative effort involving all stakeholders to find the most efficient use of the organization’s valuable resources. It will be an effort to separate the “critical few” from the “trivial many.”
